Newsletter
A First Place Mindset About Medical Error
May 31, 2016
A recent study suggests that “medical error” is the third leading cause of death in the United States. That designation has raised the issue of patient safety to greater public discourse, although a significant portion of the response to date from health care interests has been to challenge the definitions, bash the methodology, or question the numbers. But whether medical error ranks third, fourth, or 26th, CRICO and its many CRICO Strategies partners will continue their mission to be at the forefront of efforts to reduce the risks associated with patient harm.
A higher profile for medical errors should direct greater attention and resources to remedial efforts and elicit demands for “someone” to “do something” about this problem. Fortunately, many of you already are.
In every corner of health care from primary care practices to the ICU, efforts are underway to examine and improve patient safety. Armed with big data and bright ideas, the health care community has embraced patient safety improvement as a fundamental component of practice. Reducing medical errors is increasingly part of each organization’s mission and strategic plan, staffing and budgets, and education and training. More and more, Patient Safety leaderships has a seat in the C-suite and a voice in organizational governance.
For many observers, however, the numbers in the news prompt the question “Why hasn’t all of that positive effort fixed the problem?”
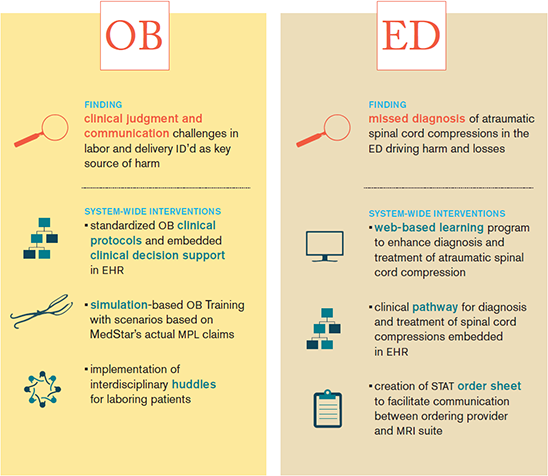
The most basic reason for that perception is that this is not a single problem. Medical errors are as diverse as the providers, patients, and settings involved. The cognitive or systemic failures that undermine care in the Emergency Room aren’t exactly the same in the OR, labor & delivery, or a pediatrician’s office. Many of your efforts have made a significant impact in key areas of risk, but no single solution—no matter how innovative—will prevent all types of medical errors. Instead, we must continue to discover and embrace solutions that make an incremental impact.
Most likely, that work won’t make headlines, but the earnest and perseverant effort to improve patient safety does make a real difference in reducing adverse events. Such progress is grounded in a deliberate and ongoing process of identification of specific vulnerabilities; comprehension of the underlying causes; and solution development, implementation, and measurement. A “slow and steady” approach probably won’t sell newspapers or generate viral tweets, but with persistence, it will make the practice of health care safer for patients and more rewarding for clinicians.
Additional Material
5 Things You Should Know About Medical Errors and Mortality
| THURSDAY, JUNE 9, 2016 |
Mind the Gaps
Avoiding the risks of communication failures in patient care
A CRICO Strategies Patient Safety Symposium | Revere Hotel, Boston, MA
Learn what you can do to avoid communication missteps that can lead to patient harm and allegations of medical malpractice.
Register Now
Latest News from CRICO
Utilization of Electronic Health Record Sex and Gender Demographic Fields: A Metadata and Mixed Methods Analysis

Establishing a Regional Registry for Neonatal Encephalopathy: Impact on Identification of Gaps in Practice