Video
Beth Felt a Lump but the Nurse Didn’t. How a Patient and her Providers Turned it Around
Dec 15, 2016
Beth Pyliotis shares her compelling story of how her breast cancer was diagnosed and treated. Despite a rocky start when a temporary NP covering for the PCP did not recommend testing and the patient insisted, the subsequent care was excellent and comprehensive once the PCP returned. See how this patient heard an apology, and now has nothing but praise for the coordination and compassion of her primary care at Atrius Health and treatment at Dana-Farber Cancer Institute.
About the Series
We’ve got you.
Our Safety Net podcast features clinical and patient safety leaders from Harvard and around the world, bringing you the knowledge you need for safer patient care.
Episodes
Recent episodes from the Safety Net series.
Bad Finger, Good Documentation
Podcast
Dec 01
A patient sued her hand surgeon, claiming the surgical approach increased the chance that their finger wouldn’t fully heal from a prior fracture. The defense leaned on contemporaneous clinical notes and documentation of the consent process to achieve a defense verdict.
Battery in Toddler’s Nose Missed at First
Podcast
Mar 28
Parents alleged that a delayed diagnosis of a foreign body in their child’s nose caused preventable nosebleeds, nasal infection, nasal septal perforation, and the need for surgery. The malpractice claim named the pediatric group, two pediatricians, and a pediatric nurse practitioner, and was settled in the low range.
Play Episode

Mar 28
A Pending Test at Discharge and a Return with Sepsis
Podcast
Jul 22
A 68-year-old male was admitted to the hospital after falling on ice and feeling short of breath. Two days after discharge, the patient arrived by ambulance at another hospital in septic shock. The patient filed a claim against the hospital, alleging that the failure to communicate a critical lab result required readmission and several weeks of follow-up treatment.
Play Episode

Jul 22
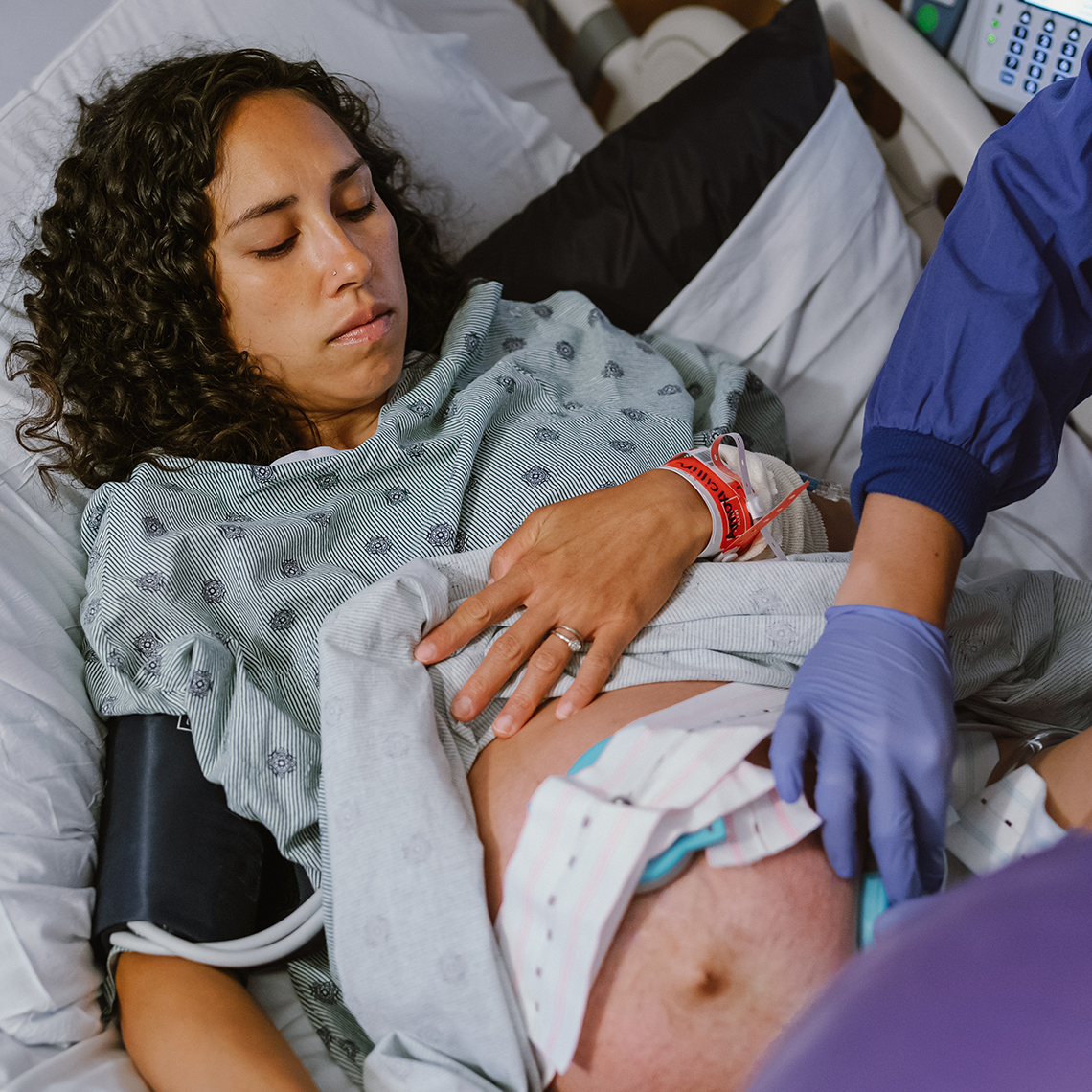
Med Error Leads to Change in L&D Policy
Podcast
May 14
A 30-year-old woman experiencing her first pregnancy, presented to the Labor and Delivery unit. She was given the wrong drug and required an emergent C-section. The “five rights” of medication administration focuses on individual factors and not necessarily on system flaws. Many organizations are also promoting just culture, which encourages reporting near-misses and patient safety events, and focuses on psychological safety and promoting a non-punitive reporting culture.
Play Episode
May 14


