Article
Testing and Results Processing
 According to CRICO’s 2014 Candello Benchmarking Report: Malpractice Risks in the Diagnostic Process, on average, a third of patients with a health complaint will undergo diagnostic testing. The ordering physicians and patients rely on the proper performance, interpretation, and transmittal of the results to reach diagnostic certainty. More than one in four of the malpractice cases in this study involved breakdowns in one or more of these testing-related steps in the diagnostic process.
According to CRICO’s 2014 Candello Benchmarking Report: Malpractice Risks in the Diagnostic Process, on average, a third of patients with a health complaint will undergo diagnostic testing. The ordering physicians and patients rely on the proper performance, interpretation, and transmittal of the results to reach diagnostic certainty. More than one in four of the malpractice cases in this study involved breakdowns in one or more of these testing-related steps in the diagnostic process.
Sending patients (or specimens) for testing is fraught with opportunities for something to go wrong. Staff, and the systems they use, have to make certain that the right patient gets the right test and safeguard that specimens are properly handled. Specialists who are, essentially, expected to be infallible in their interpretation and communication skills, need training and protocols that minimize misreads or misdirected results. Primary care providers need to ensure that their interpretations of the results align with the specialists’, and that they comprehend the full extent of the report. Together, the providers ordering and performing diagnostic tests have to guarantee that the reasons for testing are clearly expressed and that results are timely, unambiguous, and communicated in a logical format via the proper channels.
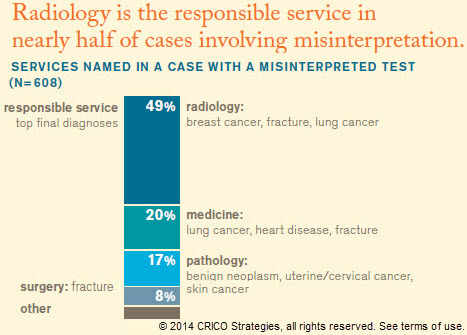
Misinterpretation of diagnostic studies is among the most common factors in failure to diagnose cases from an ambulatory setting. Hindsight provides malpractice plaintiffs with knowledge of precisely what to look for in test or lab results—or in a consultation report—leaving defendant physicians having to answer “Why didn’t you see this then?” Protocols for reducing the types of errors that most often involve test results in malpractice cases alleging a diagnostic failure need to address both interpretive accuracy and communication of results to the ordering physicians and, when appropriate, to patients directly.
Analysis of cases with breakdowns in the testing process indicate that an unflagging assumption that reported findings are thorough and accurate, or received and understood, is not a best practice.
Results inconsistent with ongoing symptoms, other findings, or trusted instincts should be questioned to better understand where to probe further along the diagnostic pathway. Physicians who accept that infallibility is unrealistic, and pursue the range of possibilities when the puzzle pieces don’t fit, are better positioned to reach an accurate and timely diagnosis and avoid allegations of malpractice.
This page is an excerpt of the full Candello report: Malpractice Risks in the Diagnostic Process.
Diagnostic Process Report Contents
Dr. Gordon Schiff talks about understanding test results. (22 sec)

Related Articles
Legal Report: Risky “Favors” for Friends