Newsletter
Starting Points for Patient Safety
Sep 29, 2016
Even if you know where you’re going, it’s harder to navigate if you don’t know where you’re starting from.
From report cards to bathroom scales to speed limits, benchmarks guide much of our lives. Whether we are comparing against a norm, peers, or ourselves, we set our goals for tomorrow based on where we are today.
One of the basic challenges for improving patient safety—after identifying the specific risks that need to be addressed—is understanding the benchmarks for improvement. What is my experience? What about my peers? What is the norm for my specialty, practice setting, geographic region, et cetera. Of course, everyone wants the number of adverse events and malpractice cases to be zero, but where along that path are you today?
Each year, CRICO’s Comparative Benchmarking System (CBS) adds more than 8,000 medical professional liability (MPL) cases from across the United States to its database. The entities that submit cases to CBS insure more than 400 hospitals and in excess of 165,000 physicians. Overall, CBS represents roughly 30 percent of the medical malpractice cases asserted in the U.S. For the time period 2010–2014, CBS offers for analysis more than 25,000 (open and closed) cases fully-coded with rigorously managed proprietary clinical coding taxonomy.
The CRICO/CBS taxonomy ensures that analysts are able to query the database across a spectrum of demographic and clinical factors that precisely pinpoint risks of statistical significance and enable credible benchmarks for comparisons both between and within health care organizations. Analyses are significantly enhanced by volume-based denominators such as the number of outpatient visits, licensed beds, inpatient days, births, or surgeries.
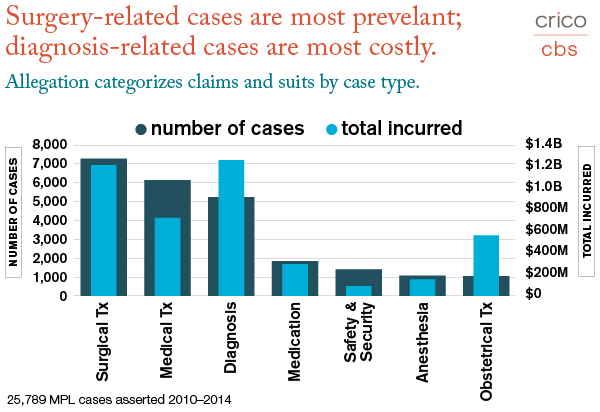
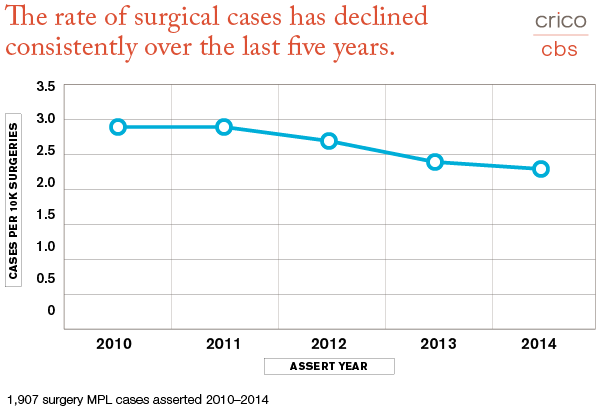
For example, while we observe that surgery-related events constitute the most common type of malpractice case (2010–2014), measuring those 7,273 cases against the total number of surgeries performed offers an alternate perspective, cases per 10,000 surgeries, which indicates a recent downward trend.
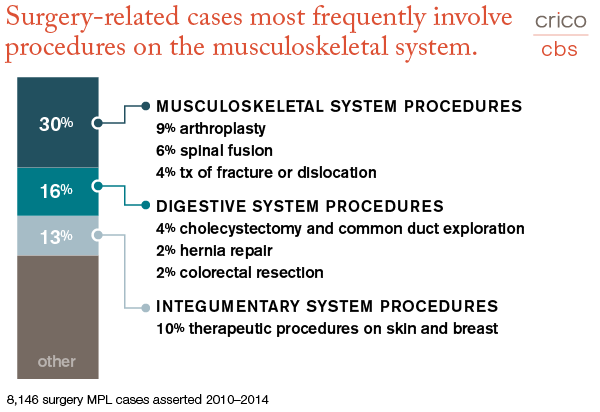
CRICO’s coding taxonomy also captures details about the location of the event (51 percent of surgery cases involve ambulatory care), the severity of the patient’s injury (63 percent are medium—non permanent—injuries) and the type of surgical procedure the claimant underwent, at both a broad and a specific level.
Across all types of health care, the power of diving deeply into an aggregated volume of malpractice cases is the ability to identify risks that might otherwise be too subtle to be detected at a single organization. The power of benchmarking is the ability to see where your organization is positioned, and to determine the strengths and weaknesses of your patient safety program. Celebrating those strengths and focusing improvement efforts on concerning outliers enables organizations to make significant strides towards zero.
Additional Materials
Latest News from CRICO
Utilization of Electronic Health Record Sex and Gender Demographic Fields: A Metadata and Mixed Methods Analysis


The Safety of Outpatient Health Care

How Informed Consent Impacts Surgery Malpractice Outcomes