Blog Post
Provider Burnout + Malpractice Risk = The Lost City of Atlantis
Did you know that a military-trained sharpshooter who is severely sleep deprived is as proficient at hitting a stationary target as when he or she is fully rested? But, did you also realize that when that target moves even slightly, that same sleep-deprived sharpshooter is only 10% as likely to hit the moving target as when he or she is fully rested?
Applied to health care, even the very best but exhausted physicians, clinicians and other providers are fully capable of delivering proficient care . . . as long as everything with the patient and in their physical environment is 100% certain, completely stable, and fully predictable so the provider can practice in a robotic way. Simply not possible.
It is interesting how long it has taken to have the word “burnout” accepted into the health care lexicon. Maybe because it triggers thoughts of weakness, vulnerability, blame, risk, abuse, and other terms that those who deliver, receive, insure or pay for healthcare don’t like to hear.
These and other aha insights and epiphanies were shared with the Candello Community by Dan Shapiro, PhD, a psychologist and Director of the Chartis Center for Burnout Solutions at our annual community summit on September 12, 2023. We were inspired to invite Dr. Shapiro to address our community after hearing him speak at the Medical Professional Liability Association (MPLA) annual meeting in New Orleans in May of 2023.
On behalf of its insured member organizations, CRICO has been deeply invested in seeking evidence and insights that could help its insureds address this ubiquitous threat to not only provider wellbeing, but also quality and safety, provider retention, and patient outcomes and satisfaction. The battlefield medicine conditions that COVID created have only accentuated and accelerated the threat that burnout poses.
Dr. Shapiro has concluded that the answer isn’t reactive gestures of appreciation or comp time for a job well done. Those are band-aids. Instead, he has seen that a systems approach to burnout offers the most hope for long-term risk reduction and for needles to move in a positive direction. For example, Chartis has seen one client save $7.4m in 12 months by facing burnout head on and retaining 160 nurses who intended to leave the organization. Similarly, another client saved $15m by reducing specialty physician turnover from 17% to 7% in one year.
It has become cliché to cite system failures as the cause of everything. For more than two decades, policymakers, academics, payers, insurers, and consultants have been saying that if we just overhaul our systems and create alignment and make leadership responsible for what those systems produce, all can be well. They are not wrong, but it’s very hard.
In the context of burnout, causes can range from poor hydration to lack of bio breaks for providers to a loss of the intrinsic reward of helping people. Believe it or not, each of the contributors to burnout does reside within a system that can be fixed, and systems are the responsibility of management.
From a medical malpractice perspective, we have developed a way to look at MPL claims and suits through a lens of burnout using our proprietary taxonomy of contributing factors (i.e., root causes). For example, we found that between 2017–22 there were 3,285 cases in the Candello database that have one or more contributing factors that map to Dr. Shapiro’s burnout “markers.” Within this cohort of cases:
- 36% involved high injury severity;
- 48% were in the ambulatory setting, 45% were inpatient, and 6% were in the emergency department;
- The three leading primary responsible services and their corresponding average indemnity payments for their cases were:
- Nursing, 640 cases with an average indemnity of $246,832
- Surgery, 486 and $234,738
- Medicine, 384 and $299,421
In this cohort of cases, the sum of the indemnity payments for these three specialties is just over $387 million.
By happenstance, we observed that the relationship between Chartis burnout factors and Candello contributing factors associated with burnout are so linear that when you literally overlay Dr. Shapiro’s factors with Candello factors, it is as if a map to the Lost City of Atlantis magically appears to guide Indiana Jones in his next adventure.
Chartis Provider Burnout Hierarchy (adjusted from Maslow’s Hierarchy)
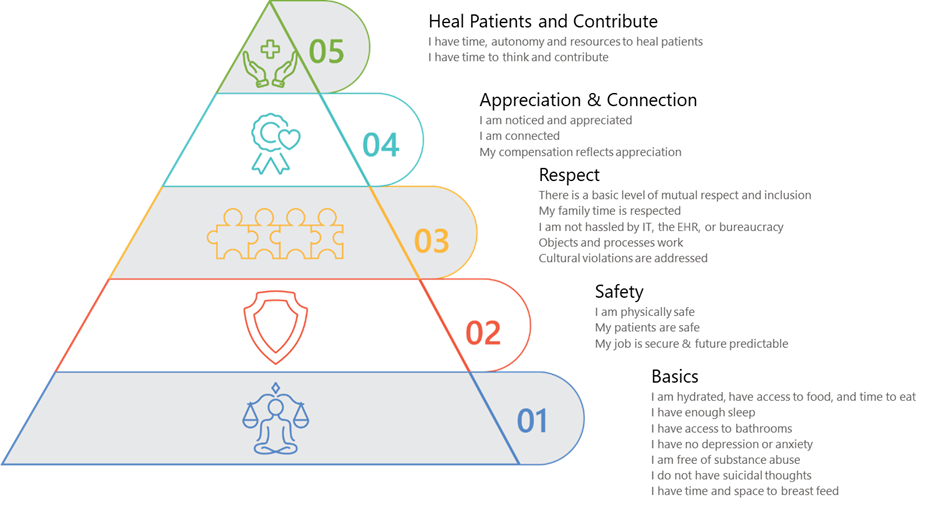
Candello Provider Burnout-related Contributing Factors
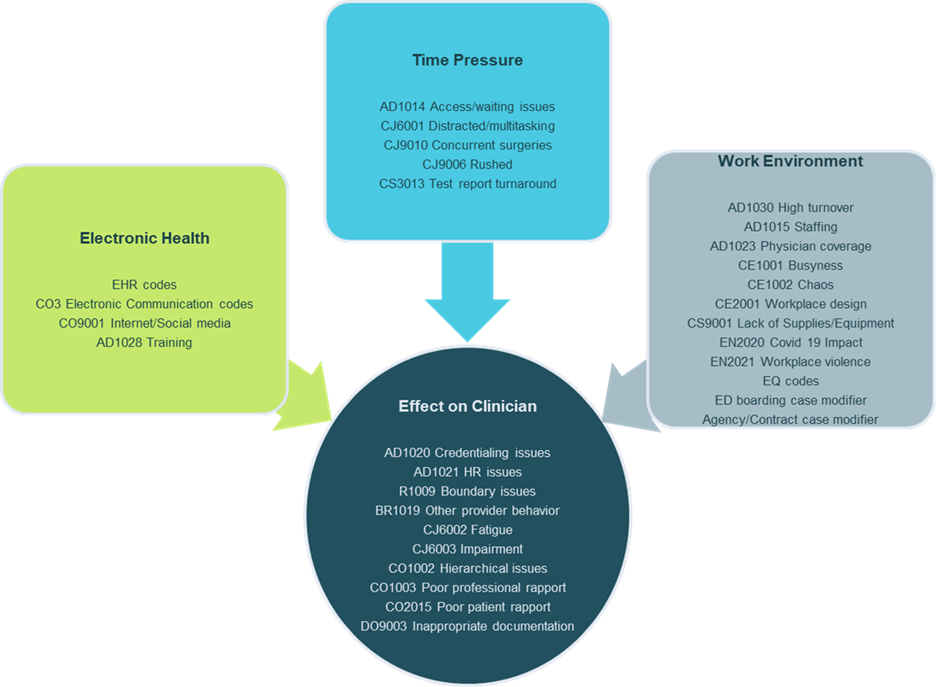
No matter what kind of data or lens on health care you might represent, a map to the Lost City of Atlantis cannot be ignored. There are too many answers and solutions to be found in this space to sit idly by as providers and their patients suffer.

To see Dr. Shapiro’s full presentation—and a trove of other proprietary content drawn from Candello’s unique national data—click to apply for a personal membership in the Candello Community, for just $400 per year. And let the discoveries begin.
Request a Community Membership

Related Blog Posts
Investing in Patient Safety


Mind the Gaps: Learning How to Avoid Miscommunication Pitfalls
January Safety Salute | MedStar Health Creating a Just Culture


