Blog Post
Addressing Race-based Algorithms in Medical Care

As a bi-racial person, this article in Becker’s Health really resonated with me. The article raises important issues of how race is addressed in medical care through the use of algorithms. These algorithms factor race into medical decisions, however they tend to look at race as a social factor rather a biological one.
One Check Box Does Not Fit All
Growing up, forms that required race usually said choose one. This always presented me with the conundrum, what do I select? While this has improved over time, there are still occasionally forms that don’t allow for selection of multiple races. As this article expresses, misidentification of race can impact quality of care.
While the article may be focused on algorithms, it touches on the overall issue of race as it relates to health care. Part of the solution is starting from the right point and properly identifying race. Some questions an organization might ask itself to address race in health care might include:
- Does your organization have a process for asking and confirming race?
- Is there a process to explain why the question is important for the patient’s health care?
- Are you prepared for scenarios where an individual may not have a full picture of their racial background?
The first step in incorporating race in health care is being able to properly have the conversations that allow us to use the information in an effective manner and not just simply rely on assumptions applied to an algorithm.
How Discrimination can Show up in MPL Claims
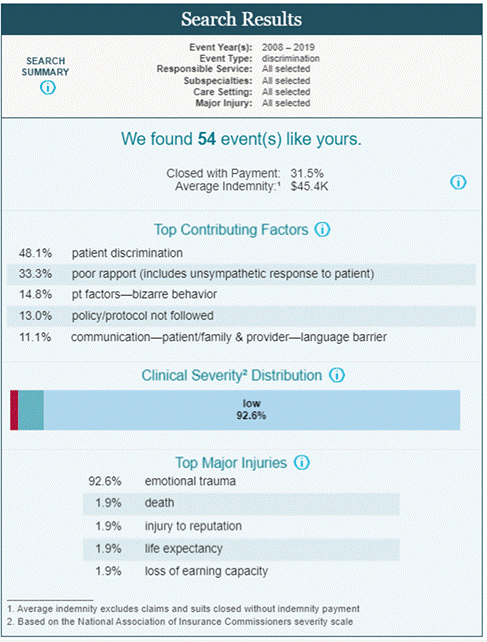
Stepping further into the impact of race on health care, is the impact of discrimination malpractice claims. A query of our national database, the Candello (previously CBS), shows that over a 10-year period, there were 54 claims that alleged discrimination. While this may seem like a few cases, we know that not all instances of discrimination result in a medical malpractice claim. As the results show, discrimination in the health care process can often lead to emotional trauma in patients. Even if an event does not lead to a medical professional liability (MPL) case, emotional trauma is still a result of inadequate care.
Continued Progress
Properly understanding the impacts of race in health care and being able to properly communicate on the topic is key to providing empathetic care. Conversations like the one in the referenced article are a good first step. I look forward to the continued progress our industry makes as it works to ensure inclusion in the practice of safe health care.
Originally published on the Candello Blog.
Related Blog Posts
Mind the Gaps: Learning How to Avoid Miscommunication Pitfalls

January Safety Salute | MedStar Health Creating a Just Culture

Diagnostic Error: The Conversation Continues

