Blog Post
Raising Awareness: Trends and Burnout
March means different things to different people. For some, it’s Lent. For others it’s Mardi Gras. And if you’re from Boston, it’s all about St. Paddy’s Day.
But for those of us working in health care, and more specifically, in the patient safety arena, March means Patient Safety Awareness Week (PSAW). Spearheaded by IHI, PSAW is an annual event which highlights safety initiatives and encourages caregivers, patients, and clinicians to reflect on how their efforts contribute to creating a safer health care environment.
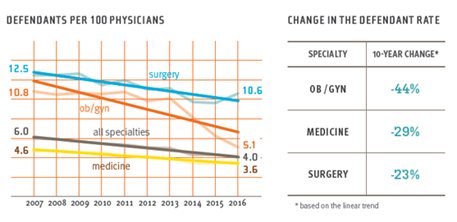
A newly published report helps raise awareness by identifying key areas of medical risk while also pinpointing areas where patient safety initiatives are having an obvious positive impact. The ten-year analysis of national malpractice claims by Candello showed a 27 percent drop (from 5.1 to 3.7) in case frequency in cases asserted per 100 physicians from 2007 to 2016.
Defendant rates declined most steeply in obstetrics/gynecology
These declines correlate with long-term safety interventions in these areas.
While case rates may be dropping, we continue to grapple with the impact physician burnout is having on patient safety. In a recently published article in NEJM Catalyst, Dr. Rich Joseph (a resident at Brigham and Women’s Hospital in Boston) takes a hard look at his own experiences and how they may be impacting his ability to safety treat patients.
“ Our ability to advocate for patients’ safety is limited by our own emotional exhaustion and separation from administrators who set the institutional policies. We strive to serve patients, yet we spend most of our days cranking the hospital’s billing machinery” —Dr. Rich Joseph, MD, MBA
As we enter Patient Safety Awareness Week, Dr. Joseph’s words resonate loudly. One particularly tragic effect of the burnout factor is how many skilled and compassionate clinicians are choosing to leave the profession entirely. So while it remains vital to focus our awareness on improved treatment options and systems risks, we also need to identify solutions which will help bring balance back into the clinical workflow, allowing more time for engagement between provider and patient.
“ ...all residents should have protected space and time to engage with the art of medicine by sitting alongside patients, rather than isolated behind a computer screen. ” —Dr. Rich Joseph, MD, MBA
We need to strengthen our resolve to avoid erasing the significant gains we've been able to achieve through our patient safety efforts by considering the myriad issues that contribute to ensuring the safest possible health care environment for our patients and for our providers; not just during PSAW, but every day, week, and year.
Related Blog Posts
Investing in Patient Safety


Mind the Gaps: Learning How to Avoid Miscommunication Pitfalls
January Safety Salute | MedStar Health Creating a Just Culture