Blog Post
Data-Driven Resources
As a researcher, I have worked extensively with an important source of malpractice data, the National Practitioner Data Bank (NPDB). Created by Congress in 1986, the NPDB is designed to serve as a central repository for paid malpractice claims, which, by law, must be reported to the NPDB. Health care organizations can query the database for information on physicians as part of the credentialing process. However, a major limitation of the NPDB as a research tool, is that it does not contain physician specialty. Serving as an exemplar of government-academic collaboration, the Federal agency that maintains the NPDB linked its NPDB data to physician specialty data contained in the AMA Physician Masterfile. This allowed our team of researchers from Brigham and Women’s Hospital and the Department of Health Care Policy at Harvard Medical School to examine national trends in malpractice at the specialty level.
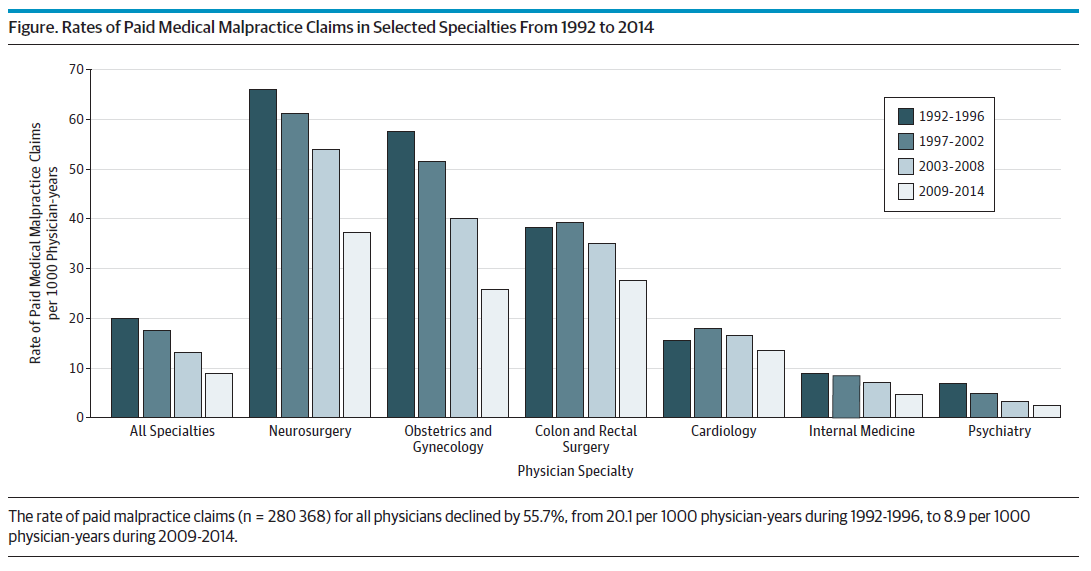
Among the key findings of this research, published online in JAMA-Internal Medicine on March 27, 2017, is that, over the period 1992 to 2014, the rate of paid malpractice claims decreased by 55.7% (from 20.1 to 8.9 per 1000 physician-years) and the mean compensation payment increased 23.3% (from $286,751 to $353,473, inflation adjusted to 2014 dollars).1
Beyond the NPDB, only a few data sources exist that enable patient safety officers and researchers to answer questions about the rates and types of medical malpractice claims. One of these is Candello Data, (previously CBS) which currently contains nearly 400,000 open and closed medical malpractice claims, representing about 30% of U.S. malpractice cases. Unparalleled in both its granularity and scope, Candello allows for a “deep dive” into the types and causes of malpractice. The contributing factors and other characteristics of malpractice cases in Candello are categorized by registered nurses who are trained as Clinical Taxonomy Specialists. Candello makes it possible for health care organizations to benchmark themselves relative to peer organizations and gain insights into their patient safety and medical liability vulnerabilities.
In my new role as Senior Clinical Analytics Specialist at CRICO, a future direction I hope to pursue is to explore how these two databases can be used in a complementary way. The combination of the detail and sophisticated taxonomy of Candello and the comprehensiveness of the NPDB should enable patient safety officers and healthcare organizations to gain the fullest possible understanding of the national landscape of medical malpractice.
1. Schaffer AC, Jena AB, Seabury SA, Singh H, Chalasani V, Kachalia A. Rates and Characteristics of Paid Malpractice Claims Among US Physicians by Specialty, 1992-2014. JAMA Intern Med. Published online March 27, 2017. doi:10.1001/jamainternmed.2017.0311
Related Blog Posts
Investing in Patient Safety


Mind the Gaps: Learning How to Avoid Miscommunication Pitfalls
January Safety Salute | MedStar Health Creating a Just Culture